Some parts of England seeing plateau in cases – Neil Ferguson
London in particular is seeing a drop in the number of positive coronavirus tests, alongside some parts of the South East and the east of England.

Some parts of England are showing a plateau in cases of Covid-19, while the rate of growth across the country as a whole is slowing, a senior epidemiologist has said.
Professor Neil Ferguson, whose early modelling of Covid-19 made him a key player in the UK’s first lockdown, said he thinks the current wave of the epidemic may be coming under control in some regions.
It comes as Health Secretary Matt Hancock said three million coronavirus vaccines have now been administered across the UK.
He tweeted that he was “delighted” with the news, adding: “We’re accelerating the Covid vaccine rollout across the UK.”
In an interview with BBC Radio 4’s Today programme, Prof Ferguson said: “I think it’s much too early to say exactly when case numbers are going to start coming down, but in some NHS regions in England and in Wales there’s sign of plateauing.”
London in particular is seeing a drop in the number of positive coronavirus tests, alongside the South East, he said.
“At the moment, it looks like in London in particular, and a couple of other regions – the South East and East of England – (that) hospital admissions may even have plateaued, though it’s hard to tell they’re coming down.
“It has to be said this is not being seen everywhere.
“Both case numbers and hospital admissions are going up in many other areas but, overall, at a national level we’re seeing the rate of growth slow.”
Prof Ferguson, who is director of the Medical Research Council’s Centre for Global Infectious Disease Analysis at Imperial College London, said he would expect to see case numbers “continue to come down slowly at a national level” but with regional variations.
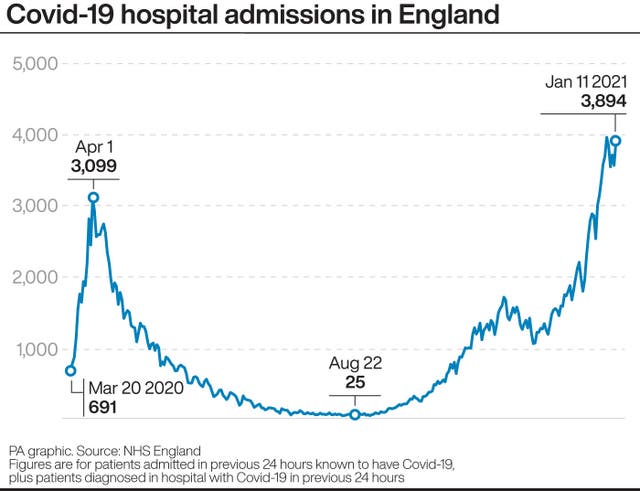
“It will take longer though for hospital admissions – daily admissions – to start coming down and even longer for hospital bed occupancy to come down,” he said.
Asked how many more weeks of rising hospital admissions and deaths the UK could be looking at, he said: “It critically depends on whether the lockdown we’re in the moment will actually control growth in all areas.
“But I would hope that hospital admissions might plateau, instead of keep going up, some time in the next week.
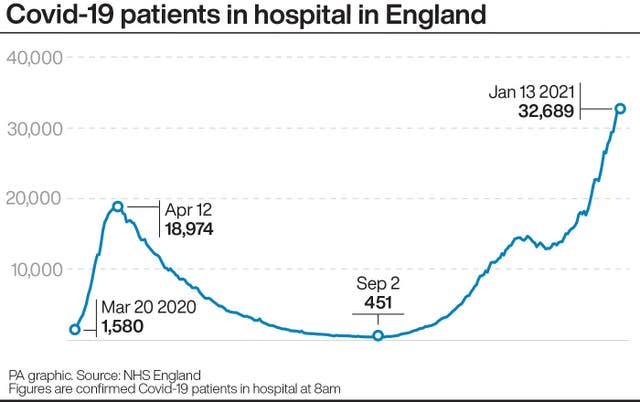
“Hospital bed occupancy may continue to rise slowly for up to two weeks and deaths maybe even for longer.
“We’re going to be well over 1,000 deaths a day, even measured by the date people die rather than the date deaths are reported, before numbers start coming down.”
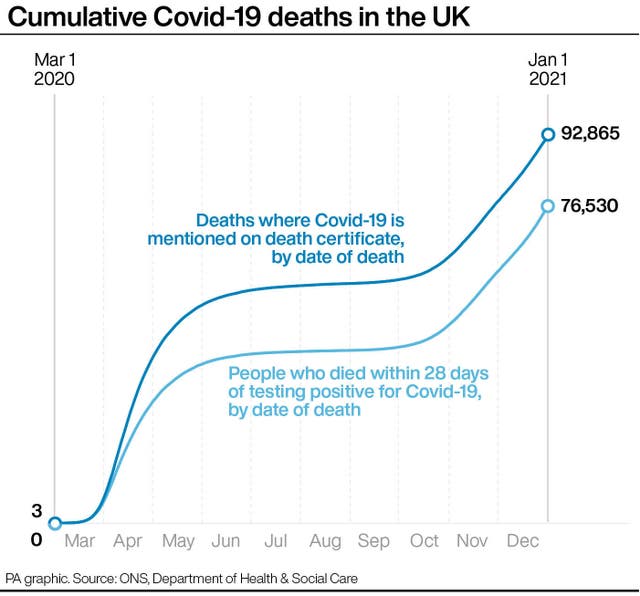
Prof Ferguson said the total number of deaths in the UK “unfortunately is going to be well over 100,000, there’s nothing we can do about that now”.
Only about 20% of the population has been infected so far, which had resulted in 100,000 deaths, he said.
“So we have to get to very high levels of vaccine coverage in those vulnerable groups before we can reduce the risk of having basically the same number of deaths again.
“If we only get up to 70% coverage in in the elderly, for instance, that still leaves 30% unprotected plus everybody else.
“We can still get a very large epidemic, which unfortunately could kill many, many people, so what the modelling and all the analysis and all the groups feeding into Sage (Scientific Advisory Group for Emergencies) says is, we need to be very cautious in how we relax restrictions and try to ensure we get as high a vaccine coverage as possible.”
Asked if there could be restrictions for many months to come, he said: “Yes, and we can’t predict all of these things in advance.
“We couldn’t have predicted this new variant coming up, but the new variant without doubt will make the relaxation of restrictions more difficult because it is substantially more transmissible.
“So it will be a gradual process to the autumn.”
Prof Ferguson suggested that the requirement to isolate after coming into contact with a person with coronavirus could be relaxed for people who have recently had the virus, such as NHS workers, but said this was “a question for policymakers”.
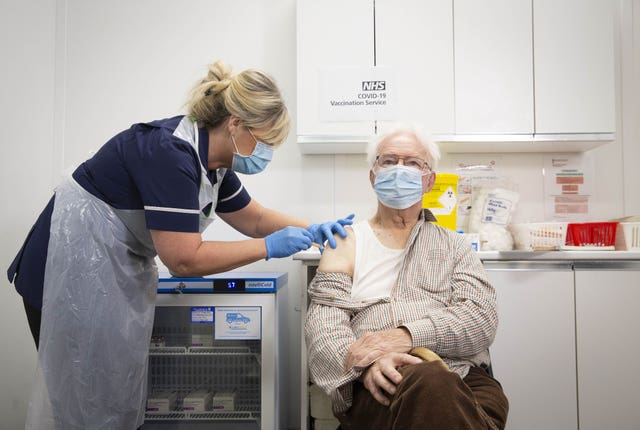
His comments came as some large high street pharmacies, including Boots and Superdrug, began rolling out Covid-19 vaccines.
Six stores across England can administer the jabs from Thursday as the Government aims to hit its target of vaccinating around 15 million of those most at-risk by mid-February.
People who are eligible for a vaccine will be contacted and invited to make an appointment through a new national booking service.
This gives them the option of having the vaccine at a pharmacy or in a GP-led vaccination centre.
Elsewhere:
– England’s deputy chief medical officer, Professor Jonathan Van-Tam, has told the Sun newspaper: “We are probably in the last few furlongs of this race, like in the Grand National. We just have a couple more fences. We have just got to stick with it.”
– Home Secretary Priti Patel again appeared confused about coronavirus rules, which say that in England someone is allowed to exercise outdoors with one other person from a different household. Ms Patel told ITV’s This Morning: “The clarity is exercising on your own and not socialising… cycling is fine, because you are on your own, you should not be cycling with other people… running, exactly in the same way, because you are on your own, walking on your own.”
– Around one in five major hospital trusts in England had no spare adult critical care beds on January 10, NHS England figures show. Some 9,267 patients also waited between 30 and 60 minutes to be handed over from ambulance teams to A&E staff in the week to January 10.
– Data leaked to the Health Service Journal (HSJ) suggests one in 10 hospital nurses are now off work in the areas of England worst affected by coronavirus. It reported the total absence rate among acute trust nurses as 9.7% as of Monday, up from around 7% at the start of December, although it is unclear exactly how many absences are linked to Covid.
Amid the warnings of struggling hospitals, the Government’s leading scientist Sir Patrick Vallance has warned the country is “in for a pretty grim period” of deaths which will not “reduce quickly”.
He told ITV’s Peston programme that high death numbers will “carry on for some weeks”.
Elsewhere, Public Health England’s Siren study found that antibodies from past infection provide 83% protection against reinfection for at least five months.
Although reinfections in people with antibodies were rare, the researchers identified 44 potential reinfections among 6,614 people who had had Covid-19 previously, putting them at risk of transmitting the virus to others.





